Continuous Glucose Monitoring

Overview of types of glucose monitoring devices and explanation of continuous glucose monitoring.
- What is glucose monitoring?
- What is continuous glucose monitoring?
- What are the prospects for an artificial pancreas?
- Points to remember
What is Glucose Monitoring?
Glucose monitoring helps people with diabetes manage the disease and avoid its associated problems. A person can use the results of glucose monitoring to make decisions about food, physical activity, and medications. The most common way to check glucose levels involves pricking a fingertip with an automatic lancing device to obtain a blood sample and then using a glucose meter to measure the blood sample's glucose level.
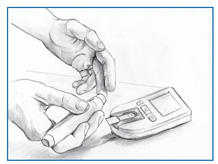
People with diabetes typically use a lancing device to obtain a blood sample and a glucose meter to measure the glucose level in the sample.
Many types of glucose meters are available, and all are accurate and reliable if used properly. Some meters use a blood sample from a less sensitive area than the fingertip, such as the upper arm, forearm, or thigh.
What is Continuous Glucose Monitoring?
Continuous glucose monitoring (CGM) systems use a tiny sensor inserted under the skin to check glucose levels in tissue fluid. The sensor stays in place for several days to a week and then must be replaced. A transmitter sends information about glucose levels via radio waves from the sensor to a pager-like wireless monitor. The user must check blood samples with a glucose meter to program the devices. Because currently approved continuous glucose monitoring devices are not as accurate and reliable as standard blood glucose meters, users should confirm glucose levels with a meter before making a change in treatment.
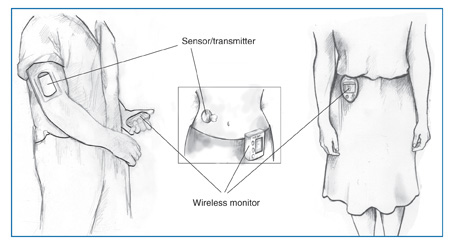
CGM systems provide glucose measurements as often as once per minute. The measurements are transmitted to a wireless monitor.
CGM systems are more expensive than conventional glucose monitoring, but they may enable better glucose control. CGM devices produced by Abbott, DexCom, and Medtronic have been approved by the U.S. Food and Drug Administration (FDA) and are available by prescription. These devices provide real-time measurements of glucose levels, with glucose levels displayed at 5-minute or 1-minute intervals. Users can set alarms to alert them when glucose levels are too low or too high. Special software is available to download data from the devices to a computer for tracking and analysis of patterns and trends, and the systems can display trend graphs on the monitor screen.
Additional CGM devices are being developed and tested. To learn more about such monitors and new products after approval, call the FDA at 1-888-INFO-FDA (463-6332) or check the FDA's website section titled "Glucose Meters & Diabetes Management".
What are the prospects for an artificial pancreas?
To overcome the limitations of current insulin therapy, researchers have long sought to link glucose monitoring and insulin delivery by developing an artificial pancreas. An artificial pancreas is a system that will mimic, as closely as possible, the way a healthy pancreas detects changes in blood glucose levels and responds automatically to secrete appropriate amounts of insulin. Although not a cure, an artificial pancreas has the potential to significantly improve diabetes care and management and to reduce the burden of monitoring and managing blood glucose.
An artificial pancreas based on mechanical devices requires at least three components:
- a CGM system
- an insulin delivery system
- a computer program that "closes the loop" by adjusting insulin delivery based on changes in glucose levels
With recent technological advances, the first steps have been taken toward closing the loop. The first pairing of a CGM system with an insulin pump—the MiniMed Paradigm REAL-Time System—is not an artificial pancreas, but it does represent the first step in joining glucose monitoring and insulin delivery systems using the most advanced technology available.
Points to Remember
- Glucose monitoring helps people with diabetes manage the disease and avoid its associated problems.
- The most common way to check glucose levels involves pricking a fingertip to obtain a blood sample and using a glucose meter to measure the glucose level in the sample.
- Continuous glucose monitoring (CGM) systems use a tiny sensor inserted under the skin to check glucose levels in tissue fluid. A transmitter sends glucose measurements to a wireless monitor.
- An artificial pancreas based on mechanical devices will consist of a CGM system, an insulin delivery system, and a computer program to adjust insulin delivery based on changes in glucose levels.
Source: NIH Publication No. 09-4551, October 2008
APA Reference
Staff, H.
(2022, January 4). Continuous Glucose Monitoring, HealthyPlace. Retrieved
on 2026, March 30 from https://www.healthyplace.com/diabetes/treatments/continuous-glucose-monitoring



